

Athlete's foot is a fungal infection that typically affects the skin between the toes but also can spread to the soles or sides of the feet. Athlete’s foot often causes itching, redness, flaking, or cracking of the skin, and the symptoms may vary depending on skin tone. In some cases, the infection can lead to painful blisters or spread to the toenails, causing further complications. Athlete's foot is often contracted in warm, damp environments like communal showers or locker rooms. People with damp or damaged skin are particularly vulnerable to this condition. A podiatrist can provide an accurate diagnosis and recommend prescription antifungal medications to address the infection and prevent it from recurring. Seeking professional care is especially important if the infection spreads or becomes severe, as untreated cases can lead to more serious issues. If you believe you have symptoms of an athlete's foot infection, it is suggested that you make an appointment with a podiatrist for a diagnosis and treatment options.
Athlete’s foot is an inconvenient condition that can be easily reduced with the proper treatment. If you have any concerns about your feet and ankles, contact Dr. Lubrina Bryant from District Podiatry, PLLC. Our doctor will treat your foot and ankle needs.
Athlete’s Foot: The Sole Story
Athlete's foot, also known as tinea pedis, can be an extremely contagious foot infection. It is commonly contracted in public changing areas and bathrooms, dormitory style living quarters, around locker rooms and public swimming pools, or anywhere your feet often come into contact with other people.
Solutions to Combat Athlete’s Foot
Athlete’s foot can cause many irritating symptoms such as dry and flaking skin, itching, and redness. Some more severe symptoms can include bleeding and cracked skin, intense itching and burning, and even pain when walking. In the worst cases, Athlete’s foot can cause blistering as well. Speak to your podiatrist for a better understanding of the different causes of Athlete’s foot, as well as help in determining which treatment options are best for you.
If you have any questions please feel free to contact our office located in Washington, D.C . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Athlete’s foot is a type of fungal infection that affects the skin on the feet. It is caused when the tinea fungus grows on the foot. It is possible to catch the fungus through direct contact with someone who has it or by touching a surface that is contaminated with it. This type of fungus thrives in warm, moist environments such as showers, locker room floors, and swimming pools. Your risk of getting it may also increase by wearing tight-fitting, closed-toe shoes, or by having sweaty feet.
Symptoms of athlete’s foot include itching, stinging or burning sensations between the toes. You may also experience toenails that are discolored, thick, crumbly, or toenails that pull away from the nail bed.
Your podiatrist may diagnose athlete’s foot by detecting these symptoms or by doing a skin test to see if there is a fungal infection present. The most common exam used to detect Athlete’s foot is a skin lesion potassium hydroxide exam. To use this method, your doctor will scrape off a small area of the infected skin and place it into potassium hydroxide. The potassium hydroxide will destroy the normal cells and leave the fungal cells untouched so that they are visible under a microscope.
There are a variety of treatment options for athlete’s foot. Some medications are miconazole (Desenex), terbinafine (Lamisil AT), clotrimazole (Lotrimin AF), butenafine (Lotrimin Ultra), and tolnaftate (Tinactin). While these options may be able to treat your fungus, it is best that you consult with a podiatrist in order to see which treatment option may work best for you.
In some cases, Athlete’s foot may lead to complications. A severe complication would be a secondary bacterial infection which may cause your foot to become swollen, painful, and hot.
There are ways that you can prevent athlete’s foot. Washing your feet with soap and water each day and drying them thoroughly is an effective way to prevent infections. You also shouldn’t share socks, shoes, or towels with other people. It is crucial that you wear shower sandals in public showers, around swimming pools, and in other public places. Additionally, you should make sure you wear shoes that can breathe and change your socks when your feet become sweaty. If you suspect that you have Athlete’s foot, you should seek help from a podiatrist as soon as possible.
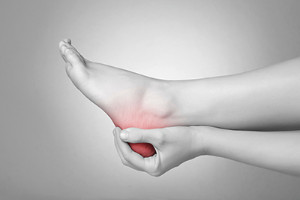
Heel pain is a widespread issue that can stem from various conditions, affecting different areas of the heel. One of the most common causes is plantar fasciitis, which occurs when the plantar fascia, a thick band of tissue running along the bottom of the foot, becomes inflamed. This condition often results in sharp pain at the bottom of the heel, particularly when taking the first steps in the morning. Another cause is heel spurs, which are bony growths that form on the heel bone, typically due to prolonged pressure or inflammation from plantar fasciitis. Heel pain can also affect the back or side of the heel. Achilles tendinitis, for example, causes pain in the back of the heel where the Achilles tendon attaches. Additionally, conditions like bursitis can lead to pain on the back or sides of the heel. If you have heel pain, it is suggested that you promptly contact a podiatrist who can accurately diagnose and offer a personalized treatment plan.
Many people suffer from bouts of heel pain. For more information, contact Dr. Lubrina Bryant of District Podiatry, PLLC. Our doctor can provide the care you need to keep you pain-free and on your feet.
Causes of Heel Pain
Heel pain is often associated with plantar fasciitis. The plantar fascia is a band of tissues that extends along the bottom of the foot. A rip or tear in this ligament can cause inflammation of the tissue.
Achilles tendonitis is another cause of heel pain. Inflammation of the Achilles tendon will cause pain from fractures and muscle tearing. Lack of flexibility is also another symptom.
Heel spurs are another cause of pain. When the tissues of the plantar fascia undergo a great deal of stress, it can lead to ligament separation from the heel bone, causing heel spurs.
Why Might Heel Pain Occur?
Treatments
Heel pain should be treated as soon as possible for immediate results. Keeping your feet in a stress-free environment will help. If you suffer from Achilles tendonitis or plantar fasciitis, applying ice will reduce the swelling. Stretching before an exercise like running will help the muscles. Using all these tips will help make heel pain a condition of the past.
If you have any questions please contact our office located in Washington, D.C . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Have you ever gotten up from a chair or out of bed in the morning, and upon taking that first step, feel like your heel has stepped on a tack? Many people experience a feeling of sharp pain which radiates into their arch from their heel and which does not allow them to put their heel on the floor. Sometimes they need to sit back down, stand only on their toes and use the wall for balance. If you can take a few steps, it seems to go away and lessen, allowing you to then resume your activity. Later, throughout your day and after a period of rest, it can happen again. If this sounds familiar you may be suffering from your first attack of heel pain.
Heel pain is a debilitating condition that affects day to day activities. Running and walking both causes stress on the heel because the heel is the part of the foot that hits the ground first. This means that the heel is taking on your entire weight. Diagnosis and treatments for heel pain can be easily found through your podiatrist.
Plantar Fasciitis
One of the main causes of heel pain is a condition known as plantar fasciitis. The plantar fascia is a band of tissue that extends along the bottom of the foot, from the toe to the bottom of the heel. A rip or tear in this ligament can cause inflammation of these tissues, resulting in heel pain. People who do not wear proper fitting shoes are often at risk of developing problems such as plantar fasciitis. Unnecessary stress from ill-fitting shoes, weight change, excessive running, and wearing non-supportive shoes on hard surfaces are all causes of plantar fasciitis.
Achilles Tendonitis
Achilles tendonitis is another cause of heel pain. Similar to plantar fasciitis, inflammation of the Achilles tendon will cause heel pain due to stress fractures and muscle tearing. A lack of flexibility of the ankle and heel is an indicator of Achilles tendonitis. If left untreated, this condition can lead to plantar fasciitis and cause even more pain on your heel.
Heel Spur
A third cause of heel pain is a heel spur. A heel spur occurs when the tissues of the plantar fascia undergo a great deal of stress, leading to a separation of the ligament from the heel bone entirely. This results in a pointed fragment of bone on the ball of the foot, known as a heel spur.

Foot pain can stem from various conditions, including plantar fasciitis, bunions, flat feet, arthritis, or injuries like sprains and fractures. Even seemingly minor discomfort can significantly impact daily activities, affecting mobility, balance, and overall quality of life. Chronic foot pain may also lead to compensation issues, causing pain in the knees, hips, or back. Ignoring persistent pain can worsen underlying conditions, making treatment more complex. Addressing foot pain begins with identifying the cause. Rest, proper footwear, and targeted stretching exercises can help in mild cases. Custom orthotics or surgical intervention may be necessary for persistent or severe pain. Early intervention is key to preventing long-term complications. If foot pain disrupts your routine, it is suggested that you consult a podiatrist for an accurate diagnosis and an effective treatment plan tailored to your needs.
Foot Pain
Foot pain can be extremely painful and debilitating. If you have a foot pain, consult with Dr. Lubrina Bryant from District Podiatry, PLLC. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Causes
Foot pain is a very broad condition that could be caused by one or more ailments. The most common include:
Diagnosis
To figure out the cause of foot pain, podiatrists utilize several different methods. This can range from simple visual inspections and sensation tests to X-rays and MRI scans. Prior medical history, family medical history, and any recent physical traumatic events will all be taken into consideration for a proper diagnosis.
Treatment
Treatment depends upon the cause of the foot pain. Whether it is resting, staying off the foot, or having surgery; podiatrists have a number of treatment options available for foot pain.
If you have any questions, please feel free to contact our office located in Washington, D.C . We offer the newest diagnostic and treatment technologies for all your foot care needs.
The feet, being the foundation of the body, carry all of the body’s weight and are therefore prone to experiencing pain and discomfort. If you are experiencing foot pain, it is important to determine where in the foot you are experiencing this pain to help discover the cause of it. While pain can be experienced virtually anywhere in the foot, the most common sites of foot pain are in the heel and ankle.
Heel pain can be due to a multitude of conditions including plantar fasciitis, Achilles tendinitis, and heel spurs. Pain experienced in the ankle can be a sign of an ankle sprain, arthritis, gout, ankle instability, ankle fracture, or nerve compression. In more serious cases, pain in the foot can be a sign of improper alignment or an infection.
Foot pain can be accompanied by symptoms including redness, swelling, stiffness and warmth in the affected area. Whether the pain can be described as sharp or dull depends on the foot condition behind it. It is important to visit your local podiatrist if your foot pain and its accompanying symptoms persist and do not improve over time.
Depending on the location and condition of your foot pain, your podiatrist may prescribe certain treatments. These treatments can include but are not limited to prescription or over-the-counter drugs and medications, certain therapies, cortisone injections, or surgery.
If you are experiencing persistent foot pain, it is important to consult with your foot and ankle doctor to determine the cause and location. He or she will then prescribe the best treatment for you. While milder cases of foot pain may respond well to rest and at-home treatments, more serious cases may take some time to fully recover.
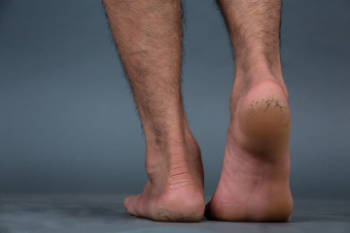
Cracked heels can be uncomfortable and unsightly, and vitamin deficiencies may contribute to their development. Insufficient levels of certain vitamins, especially from the B-vitamin group, can cause the skin to become dry and brittle, leading to cracks. Vitamin B1, also known as thiamine, plays a key role in maintaining healthy skin, and a deficiency can result in rough, cracked skin on the feet. Vitamin B3, or niacin, helps the skin retain moisture and improve its elasticity, preventing cracks. Vitamin B6 supports the body's ability to repair damaged tissues, including the skin, while vitamin B12 is vital for maintaining skin health and preventing dryness. A lack of these vitamins can impair the skin’s ability to stay hydrated and repair itself, making the heels more prone to cracking. If you have developed cracked heels, it is suggested that you contact a podiatrist who can effectively treat this condition.
Cracked heels are unsightly and can cause further damage to your shoes and feet. If you have any concerns, contact Dr. Lubrina Bryant from District Podiatry, PLLC. Our doctor can provide the care you need to keep you pain-free and on your feet.
Cracked Heels
Cracked heels appear unappealing and can make it harder for you walk around in sandals. Aside from looking unpleasant, cracked heels can also tear stockings, socks, and wear out your shoes. There are several methods to help restore a cracked heel and prevent further damage.
How Do You Get Them?
Dry skin is the number one culprit in creating cracked heels. Many athletes, walkers, joggers, and even swimmers suffer from cracked heels. Age and skin oil production play a role to getting cracked heels as well.
Promote Healing
Over the counter medicines can help, especially for those that need instant relief or who suffer from chronic dry feet.
Wear Socks – Wearing socks with medicated creams helps lock in moisture.
Moisturizers – Applying both day and night will help alleviate dryness which causes cracking.
Pumice Stones – These exfoliate and remove dead skin, which allows for smoother moisturizer application and better absorption into the skin.
Change in Diet
Eating healthy with a well-balanced diet will give the skin a fresh and radiant look. Your body responds to the kinds of food you ingest. Omega-3 fatty acids and zinc supplements can also revitalize skin tissue.
Most importantly, seek professional help if unsure how to proceed in treating cracked heels. A podiatrist will help you with any questions or information needed.
If you have any questions, please feel free to contact our office located in Washington, D.C . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Cracked heels may make you want to think twice about showing off your feet in warmer weather. However, cracked heels may be harmful to more than just the appearance of your feet. If deep fissures and cracks develop in your heels, they may make walking and standing painful for you. Additionally, these openings make way for germs to enter through your skin and cause infection.
There are several different causes of cracked heels. One of the most common reasons for this ailment is dry skin. This problem may make your keeps feel rough tight and itchy. Dry skin may be caused by cold air, extremely hot water, harsh soaps, and aging. Skin disorders such as eczema and psoriasis may eventually lead to dry skin. In some cases, complications may arise from cracked heels. Some of these complications are a loss of feeling in the heel, cellulitis, or a diabetic foot ulcer.
There are ways you can try to prevent getting cracked heels. One of the best ways to do so is to avoid wearing flip flops and sandals because these shoes increase your risk of drying out your feet. You should also avoid wearing shoes with a tall skinny heel, because these shoes cause your heel to expand sideways. At night, you should slather on a thick moisturizing cream on your feet and then cover them in socks to keep your feet moisturized overnight. Drinking water to stay hydrated is also a good way to ensure that your skin doesn’t become dry.
If you suffer from a severe case of cracked feet, you should make an appointment with your podiatrist to see what treatment methods are best for you.
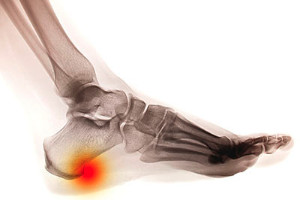
Heel spurs are bony growths that develop on the underside of the heel bone, typically as a result of prolonged stress or strain on the foot. The most common cause of heel spurs is plantar fasciitis, an inflammation of the tissue that connects the heel to the toes. Other factors that contribute to heel spurs include wearing improper footwear, obesity, repetitive activities that put pressure on the feet, and abnormal foot mechanics such as flat feet or high arches. While heel spurs themselves are often painless, they can lead to complications such as chronic pain, difficulty walking, and inflammation. In some cases, the spur may press on nearby nerves, causing sharp or shooting pain. If left untreated, heel spurs may limit mobility and interfere with daily activities, leading to long-term discomfort and reduced quality of life. If you have heel pain, it is suggested that you consult a podiatrist who can provide an accurate diagnosis and treatment solutions.
Heel spurs can be incredibly painful and sometimes may make you unable to participate in physical activities. To get medical care for your heel spurs, contact Dr. Lubrina Bryant from District Podiatry, PLLC. Our doctor will do everything possible to treat your condition.
Heels Spurs
Heel spurs are formed by calcium deposits on the back of the foot where the heel is. This can also be caused by small fragments of bone breaking off one section of the foot, attaching onto the back of the foot. Heel spurs can also be bone growth on the back of the foot and may grow in the direction of the arch of the foot.
Older individuals usually suffer from heel spurs and pain sometimes intensifies with age. One of the main condition's spurs are related to is plantar fasciitis.
Pain
The pain associated with spurs is often because of weight placed on the feet. When someone is walking, their entire weight is concentrated on the feet. Bone spurs then have the tendency to affect other bones and tissues around the foot. As the pain continues, the feet will become tender and sensitive over time.
Treatments
There are many ways to treat heel spurs. If one is suffering from heel spurs in conjunction with pain, there are several methods for healing. Medication, surgery, and herbal care are some options.
If you have any questions feel free to contact our office located in Washington, D.C . We offer the latest in diagnostic and treatment technology to meet your needs.