Juvenile idiopathic arthritis, or JIA, is a type of arthritis that affects children and adolescents. The exact cause is unknown, but it is believed to result from a combination of genetic and environmental factors that trigger an autoimmune response. In JIA, the immune system mistakenly attacks the joints, causing inflammation and pain. The condition can affect one or multiple joints, often leading to swelling, stiffness, and limited movement. Common symptoms include joint pain, especially in the morning, fever, and fatigue. Some children may also experience growth problems and eye inflammation. JIA can be classified into different types based on the number of joints affected and other features. If your child’s feet are affected by any of the above symptoms, it is suggested that you consult a podiatrist who can provide the necessary care for relief.
Making sure that your children maintain good foot health is very important as they grow. If you have any questions, contact Dr. Lubrina Bryant of District Podiatry, PLLC. Our doctor can provide the care you need to keep you pain-free and on your feet.
Keeping Children's Feet Healthy
Having healthy feet during childhood can help prevent medical problems later in life, namely in the back and legs. As children grow, their feet require different types of care. Here are some things to consider...
Although babies do not walk yet, it is still very important to take care of their feet.
Avoid putting tight shoes or socks on his or her feet.
Allow the baby to stretch and kick his or her feet to feel comfortable.
As a toddler, kids are now on the move and begin to develop differently. At this age, toddlers are getting a feel for walking, so don’t be alarmed if your toddler is unsteady or ‘walks funny’.
As your child gets older, it is important to teach them how to take care of their feet.
Show them proper hygiene to prevent infections such as fungus.
Be watchful for any pain or injury.
Have all injuries checked by a doctor as soon as possible.
Comfortable, protective shoes should always be worn, especially at play.
If you have any questions please feel free to contact our office located in Washington, D.C . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.

Stretching the feet and ankles is essential for preventing running injuries and maintaining flexibility. One exercise involves picking up small objects like marbles or coins with the toes, strengthening the foot muscles and improving coordination. Single-leg balancing on a ball enhances stability by engaging the ankle and foot muscles, which reduces the risk of sprains. Plantar stretching helps loosen the plantar fascia, which can become tight from repetitive impact. This can be done by pulling the toes back gently or rolling the foot over a frozen water bottle to relieve tension. Incorporating these stretches into a regular routine helps improve strength, flexibility, and balance. If you have sustained a foot or ankle injury while running, it is suggested that you consult a podiatrist who can treat various foot conditions, and guide you on additional running injury prevention tips.
All runners should take extra precaution when trying to avoid injury. If you have any concerns about your feet, contact Dr. Lubrina Bryant of District Podiatry, PLLC. Our doctor will treat your foot and ankle needs.
How to Prevent Running Injuries
There are a lot of mistakes a runner can make prior to a workout that can induce injury. A lot of athletes tend to overstretch before running, instead of saving those workouts for a post-run routine. Deep lunges and hand-to-toe hamstring pulls should be performed after a workout instead of during a warmup. Another common mistake is jumping into an intense routine before your body is physically prepared for it. You should try to ease your way into long-distance running instead of forcing yourself to rush into it.
More Tips for Preventing Injury
If you have any questions, please feel free to contact our office located in Washington, D.C . We offer the newest diagnostic and treatment technologies for all your foot care needs.
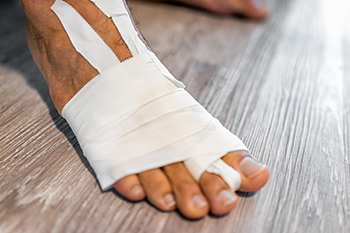
Turf toe sounds like a sports injury, but it can happen to anyone. This painful sprain of the big toe joint happens when the toe bends too far upward, overstretching the ligaments. Athletes on artificial turf are common victims, but so are yogis, dancers, and even people tripping on stairs. A simple misstep in flexible shoes can do it. At first, it may feel like a mild ache, but swelling and stiffness quickly set in, making it hard to push off when walking. Without rest, it can linger, turning a minor sprain into a chronic problem. Relief includes taping and wearing stiff-soled shoes to limit movement. Severe cases may require targeted exercises or surgery. If your big toe hurts after an awkward bend, it is suggested that you schedule an appointment with a podiatrist for a proper diagnosis and appropriate treatment.
Toe pain can disrupt your daily activities. If you have any concerns, contact Dr. Lubrina Bryant of District Podiatry, PLLC. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Causes Toe Pain?
Most severe toe pain is caused due to a sports injury, trauma from dropping something heavy on the toe, or bumping into something rigid. Other problems can develop over time for various reasons.
Toe pain can be caused by one or more ailments. The most common include:
When to See a Podiatrist
Diagnosis
In many cases the cause of toe pain is obvious, but in others, a podiatrist may want to use more advanced methods to determine the problem. These can range from simple visual inspections and sensation tests to X-rays and MRI scans. Prior medical history, family medical history, and any recent physical traumatic events will all be taken into consideration for a proper diagnosis.
Treatment
Treatments for toe pain and injuries vary and may include shoe inserts, padding, taping, medicines, injections, and in some cases, surgery. If you believe that you have broken a toe, please see a podiatrist as soon as possible.
If you have any questions please feel free to contact our office located in Washington, D.C . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
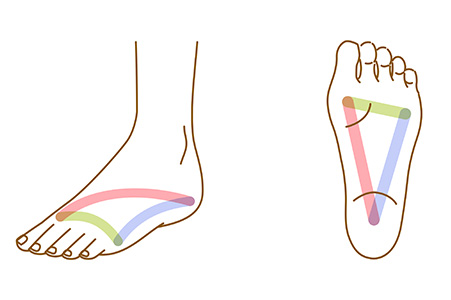
The arches of the foot play a significant role in movement, stability, and shock absorption. The foot has three arches, the medial longitudinal arch, the lateral longitudinal arch, and the transverse arch. These structures are formed by the tarsal and metatarsal bones and are supported by ligaments and tendons. The medial arch, which is the highest and most flexible, distributes weight and adapts to changes in terrain. The lateral arch is lower and provides stability, while the transverse arch helps maintain foot shape and balance. A well-functioning arch system allows efficient weight distribution and reduces strain on the joints. However, arch abnormalities can lead to pain and dysfunction. A low arch, or flat foot, often results in excessive foot pronation, which increases the risk of heel pain and arch discomfort. A high arch may reduce shock absorption, placing excessive pressure on the forefoot and heel. A podiatrist can evaluate your foot’s arch structure, diagnose potential issues, and provide treatment options like custom orthotics, or, in severe cases, surgery. If you are experiencing pain in the arch of your foot, it is suggested that you schedule an appointment with a podiatrist for an exam, diagnosis, and treatment options.
If you have any concerns about your feet, contact Dr. Lubrina Bryant from District Podiatry, PLLC. Our doctor can provide the care you need to keep you pain-free and on your feet.
Biomechanics in Podiatry
Podiatric biomechanics is a particular sector of specialty podiatry with licensed practitioners who are trained to diagnose and treat conditions affecting the foot, ankle and lower leg. Biomechanics deals with the forces that act against the body, causing an interference with the biological structures. It focuses on the movement of the ankle, the foot and the forces that interact with them.
A History of Biomechanics
Modern technological improvements are based on past theories and therapeutic processes that provide a better understanding of podiatric concepts for biomechanics. Computers can provide accurate information about the forces and patterns of the feet and lower legs.
Understanding biomechanics of the feet can help improve and eliminate pain, stopping further stress to the foot.
If you have any questions please feel free to contact our office located in Washington, D.C . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.